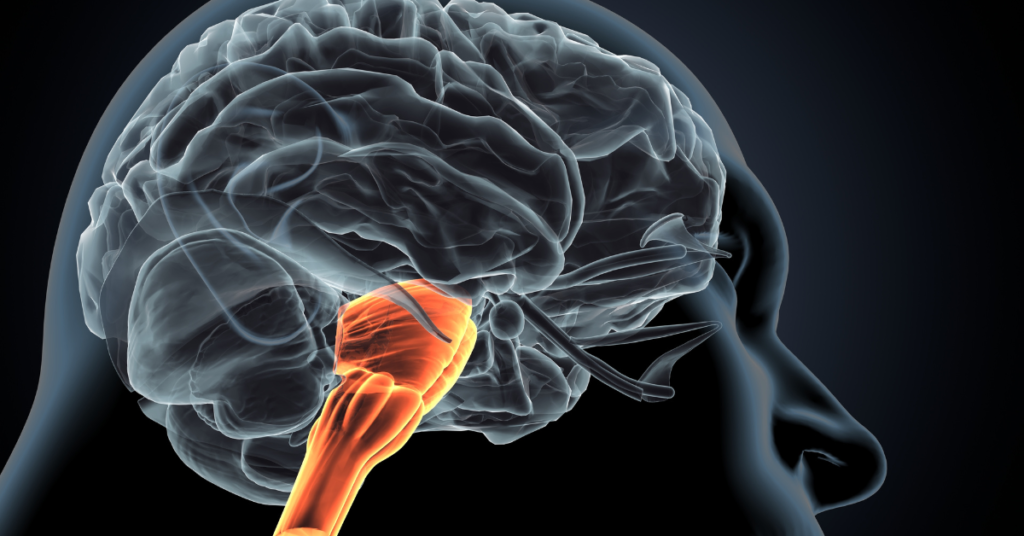
The nervous system is made up of two main components: the central nervous system, which consists of the brain and the spinal cord, and the peripheral nervous system, which consists of nerve cells that branch off the spinal cord and connect the central nervous system to the rest of the body. To execute daily functions, the nervous system relies on constant communications between the central and peripheral nervous systems to relay information from the body to the brain and vice versa. One important area connecting the central and peripheral nervous systems is the part of the brain attached to the spinal cord, called the medulla oblongata.
The medulla oblongata is located at the base of your brain just below the pons, making up the lowest part of the brainstem (Figure 1) and sitting right at the opening at the bottom of the skull.
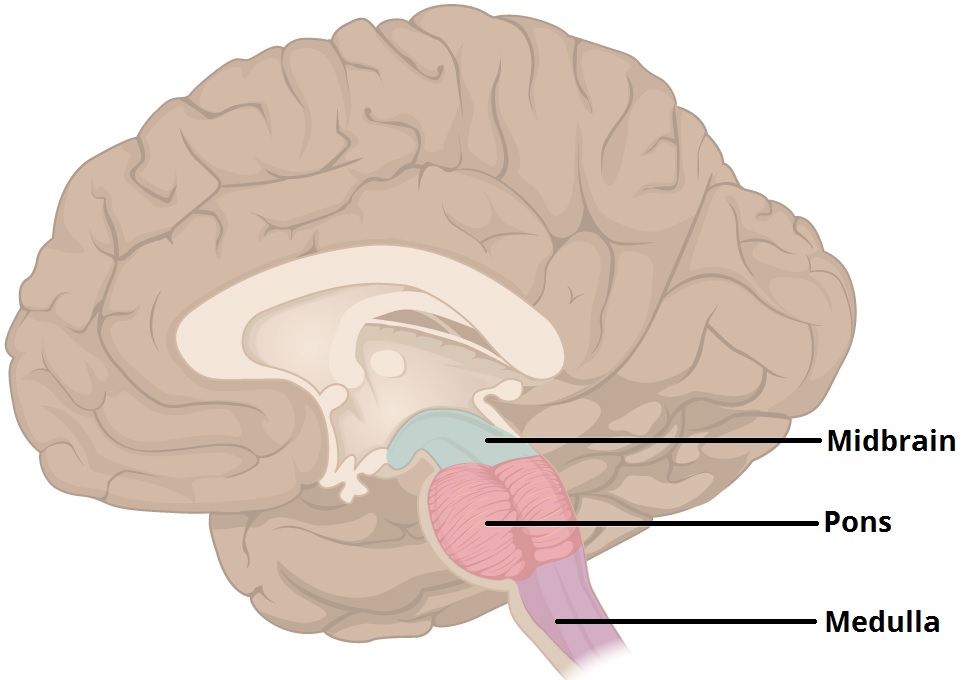
Figure 1. The three major parts of the brainstem. In purple is the Medulla Oblongata. Image by OpenStax College [CC BY 3.0], via Wikimedia Commons
The medulla oblongata is a small yet vital structure that plays a key role in controlling involuntary functions, including breathing, digestion, heart rate, and body temperature regulation. Exiting through the medulla oblongata are four pairs of cranial nerves, which — unlike other nerves — emerge directly from the brain instead of the spinal cord to reach different parts of the body. These four pairs of cranial nerves carry out a range of functions, mainly related to motor control of the upper digestive system and sensory feedback from the heart and the digestive system, which are important for involuntary functions.
Because of the medulla oblongata’s vital position connecting the spinal cord to the brain and its role in essential life functions, damage to this region can cause debilitating diseases. The cause of the injury can range from physical trauma to blood supply disruption, such as a stroke or haemorrhage. The two major syndromes associated with the medulla oblongata are medial medullary syndrome and lateral medullary syndrome, both of which are forms of stroke that affect different regions of the medulla oblongata. Common symptoms of medial medullary syndrome include upper and lower limb paralysis, whereas lateral medullary syndrome involves impaired pain and thermal sensation. Disrupted communication between the brain and the spinal cord can also cause ataxia symptoms, including nystagmus and gait ataxia.
Clinically, measuring changes in the volume of the medullar oblongata and other brain regions through magnetic resonance imaging can provide valuable information about the degree of neurodegeneration and disease progression. The volume of the medulla oblongata may also serve as a biomarker of spinal cord damage and clinical disability in multiple sclerosis. Volume decrease of the medulla oblongata has been observed in SCA1, SCA2, SCA3, and even pre-ataxic SCA3 patients, making the pathology a possible biomarker for these diseases. However, the change in volume was not observed in pre-ataxic SCA2 patients or SCA6 patients, indicating that it is not a universal marker for all ataxias.
Overall, the medulla oblongata plays an essential role in our daily functions and could serve as a biomarker for many neurological diseases. However, the link between the abnormalities of the medullar oblongata and SCA is still under investigation.
If you would like to learn more about the medulla oblongata, take a look at this article by the Cleveland Clinic.
Snapshot Written by: Christina (Yi) Peng
Edited by: Sarah Donofrio

Snapshot: What Are Silent Mutations?
Our DNA (deoxyribonucleic acid) serves as a genetic blueprint for building and maintaining our tissues. This complex molecule contains the information needed to build proteins, written in a code made Read More…

Snapshot: What is a Variant of Uncertain Significance (VUS)?
What is a variant? The human genome contains over 3 billion base pairs– individual “letters” in the DNA code that make the instructions for our cells and bodies to function. Read More…

Snapshot: What Are Nonsense Mutations?
Our DNA (deoxyribonucleic acid) serves as a genetic blueprint for building and maintaining our tissues. This complex molecule contains the information needed to build proteins, written in a code made Read More…



