Join our free Let’s Move Exercise Program! Accessible, expert-led virtual sessions to help you build strength and improve balance from home. REGISTER
Join our free Let’s Move Exercise Program! Accessible, expert-led virtual sessions to help you build strength and improve balance from home. REGISTER
Ataxia is a degenerative disease of the nervous system. Many symptoms of Ataxia mimic those of being drunk, such as slurred speech, stumbling, falling, and incoordination. These symptoms are caused by damage to the cerebellum, the part of the brain that is responsible for coordinating movement. Ataxia treatment involves a combination of medication to treat symptoms and therapy to improve quality of life, but there is no magic cure for the disease.
People affected by Ataxia may experience problems with using their fingers and hands, arms, legs, walking, speaking or moving their eyes. Ataxia affects people of all ages. Age of symptom-onset can vary widely, from childhood to late-adulthood. Complications from the disease are serious and oftentimes debilitating. Some types of Ataxia can lead to an early death.
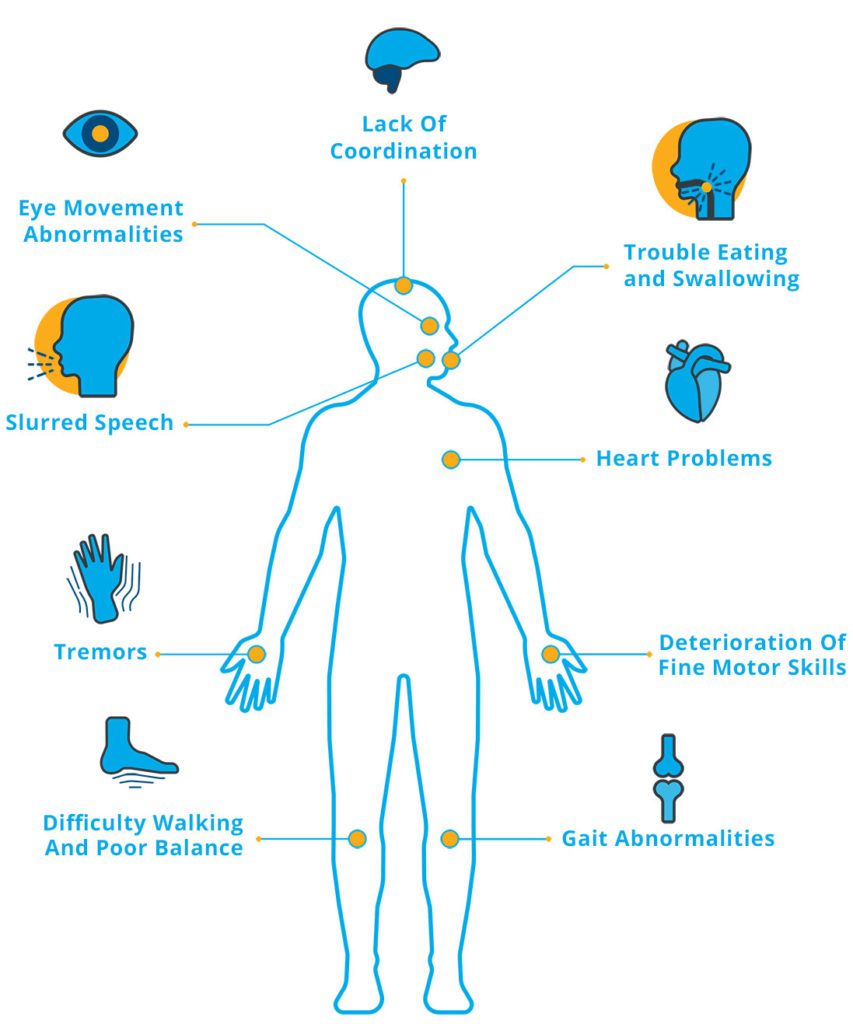
Ataxia symptoms vary by person and type of Ataxia. Rate of progression varies as well. Symptoms may worsen slowly, over decades – or quickly, over mere months. Common symptoms of Ataxia are:
Individuals with Ataxia often require the use of wheelchairs, walkers, and/or scooters to aid in their mobility.
Ataxia is diagnosed using a combination of strategies that may include medical history, family history, and a complete neurological evaluation. Various blood tests may be performed to rule out other disorders. Genetic blood tests are available for many types of hereditary Ataxia.
Taking an active role and advocating for patient needs is important when seeking an Ataxia diagnosis. Begin with a discussion with a primary care physician. However, some physicians may not be familiar with Ataxia because it is a rare disease. If Ataxia is suspected, the primary care physician will likely make a referral to a neurologist. Neurologists will have the expertise needed to confirm a diagnosis and determine the type of Ataxia. NAF maintains a list of neurologists that are familiar with Ataxia. This list is a good starting place to look for neurologists that have experience working with Ataxia patients. Gather the following information before a neurologist appointment:
Receiving a diagnosis of Ataxia can be overwhelming. It might feel like there is nothing you can do – but there is! We have resources to get you started on your journey. Learn, join the network of support, and get involved in making a difference. Here are some things that you can do:
The goal of Ataxia treatment is to improve the quality of life and requires an individualized approach. It is important to work closely with a neurologist to develop a plan to address symptoms. Speech and language therapy, occupational therapy, and physical therapy are common treatment options. They are sometimes used in conjunction with medication therapy to manage symptoms. Many research efforts are currently underway to find more effective treatments for Ataxia. Become a member of NAF to receive news when new treatment options become available. Watch our webinars about Ataxia for more information.
Staying active for as long as possible is an important part of the treatment plan for people with Ataxia. Consult with your physician, neurologist or physical therapist before starting an exercise regimen. Read “11 Exercises for Ataxia Patients,” for things that can be done at home to help maintain strength and balance.
Common symptoms associated with Ataxia are listed below with the off-label medications that have been used to treat them. These medications have been reported in medical literature or by Ataxia clinicians. The generic name is listed first (if one is available) with the brand name in parentheses.
NAF provides support and funding to the world’s greatest Ataxia scientists. We continue to collaborate with top researchers, looking for better treatment options and a cure. Learn more about current research opportunities and clinical trials for Ataxia on our research page.
NAF Support Groups are social gatherings that allow you to connect with others affected by Ataxia and learn more about living with the disease. Check out our event calendar for a list of upcoming meetings or find a Support Group Leader in your area to contact them directly. They’d love to hear from you!
We also have ambassadors in some areas that do not have support groups. These are local volunteers that welcome you to reach out to them with questions. There are online support group options as well.
Hereditary Ataxias are genetic, which means they are caused by a defect in a certain gene that is present from the start of a person’s life, inherited from your parents. Hereditary Ataxias can be divided into those that are dominantly inherited, passing from generation to generation due to a single copy of a defective gene passing from parent to child, and those that are recessively inherited, Ataxia seen in a single generation and is due to two copies of a defective gene; one passed from each parent (who are carriers) to the child.
Each child of a parent with an autosomal dominant Ataxia gene has a 50% chance of inheriting the Ataxia gene. Since the gene is dominant, if a gene is passed on to the child from one parent, the child will develop the disease. Men and women are affected equally.
Spinocerebellar Ataxia
Spinocerebellar Ataxia is one specific type of Ataxia among a group of inherited diseases of the central nervous system. Genetic defects lead to impairment of specific nerve fibers carrying messages to and from the brain resulting in degeneration of the cerebellum (the motor coordination center of the brain). With the advancement of research more than 40 different genes of SCA have been found with SCA 1 being the first to be found.
Watch a video about Spinocerebellar Ataxia
Episodic Ataxia
Episodic Ataxia is clinically characterized by attacks of Ataxia with a clear onset of resolution. There are now eight recognized episodic Ataxia syndromes, numbered 1-8, in addition to late onset episodic Ataxia. The genes are known for EA1, EA2, ES5, and EA6. The best characterized are EA1 and EA2, the others are exceptionally rare and largely defined by single families.
Autosomal recessive inherited diseases affect males and females equally, but both parents must be carriers of the Ataxia gene and each must pass on the Ataxia gene to the child for the child to develop the disease. Each child of parents who are carriers of a recessive gene have a 25% chance of developing the disease, a 50% chance of inheriting just one of the Ataxia genes, becoming a carrier themselves, and a 25% chance of inheriting no Ataxia genes. Because a single recessive Ataxia gene does not cause symptoms, it can be passed on in a family for generations without being recognized. Therefore, there can appear to be no “family history” of Ataxia if the disease was inherited as a recessive gene.
Friedreich’s Ataxia
Friedreich Ataxia (FRDA) was named after Nikolaus Friedreich, who first described it in 1863. It was the first form of hereditary Ataxia to be distinguished from other forms of Ataxia. It is caused by an abnormality of a single gene called the Frataxin (FXN) gene. The abnormality can be passed from generation to generation by family members who carry it. Two copies of each gene are inherited; one copy from the mother and one copy from the father. An individual who has one copy of an altered or nonfunctioning FXN gene does not develop any neurological symptoms and is called a carrier.
Ataxia Telangiectasia
Ataxia Telangiectasia appears early in childhood when children begin to walk. Though they usually start walking at a normal age, they wobble or sway when walking, standing still or sitting. They start to show signs of Ataxia and soon after will show sign of “telangiectasia,” or tiny red “spider” veins, which appear in the corners of the eyes or on the surface of the ears and cheeks exposed to sunlight. This unique appearance together with ataxia is what led to naming this disease “ataxia-telangiectasia.”
Mitochondrial Ataxia
Ataxia can be inherited in other ways too. Mitochondrial Ataxias pass from mother to child through the defect Mitochondria in the mother’s eggs.
There is a large group of people who have symptoms of Ataxia that usually begin in adulthood, appear “out of nowhere”, and who have no known family history of the disease. With acquired Ataxia, there is an external cause, which means a person developed it because of something that happened during their life. This can include many different problems and events such as vitamin deficiencies, autoimmune conditions, some infections, exposure to toxic substances or drugs (especially alcohol), various cancers, stroke, traumatic brain injury, and many more.
Physicians often use various terms when they make a diagnosis of Sporadic Ataxia. Some of those terms include:
Multiple System Atrophy (MSA)
In some people, the symptoms of Sporadic Ataxia are a prelude to the development of Multiple System Atrophy (MSA), which includes Ataxia, Parkinsonian features (such as rigidity and slowness of movement), and difficulty with the autonomic nervous system. The autonomic nervous system controls the automatic functioning of the body, including regulation of blood pressure, digestion, bladder and bowel function, some sexual functions, and sweating. People with MSA, whose symptoms begin with Sporadic Ataxia, may develop Parkinsonian symptoms of slowness and stiffness of movement along with difficulty turning over in bed and rising from a soft chair.
We encourage those affected by Ataxia, family members, caregivers, and friends to get involved in the search for a cure. This can include participating in research initiatives and clinical trials that are working towards new treatments, staying connected with others that have Ataxia, and/or organizing fundraisers to support NAF’s work.
