
Written by Poojashree Chettiar
Edited by Pragya Goel, PhD
AI and wearable tech may transform how ataxia is monitored
Could everyday devices help track ataxia?
Finding treatments for neurological disorders like spinocerebellar ataxias (SCAs) and multiple system atrophy (MSA-C) has been challenging. A major reason is the lack of good tools to sensitively measure if a patient’s condition is getting worse, which is crucial for therapeutic development and clinical trials.
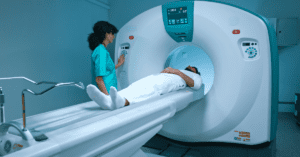
Most of us already wear watches or fitness trackers that count steps, measure heart rate, or remind us to move. But what if similar technology could be used beyond the clinic to precisely monitor subtle changes in motor behaviors that are impacted in SCAs and MSA-C?
Both SCAs and MSA-C affect the cerebellum, the part of the brain that coordinates balance and movement. Thus, patients experience trouble in walking, balance, coordination, speaking and swallowing. For years, doctors have measured symptoms using rating scales like the Scale for the Assessment and Rating of Ataxia (SARA). While helpful, these exams only capture a “snapshot” during clinic visits and may miss subtle changes in daily life. They also rely on the neurologist’s judgment, which can vary and may not fully reflect a person’s lived experience. This is the gap that Manohar and colleagues set out to address. They tested whether wearable sensors, similar to everyday fitness trackers, could provide a more sensitive and reliable way to track ataxia progression in the real world.
How the Study Worked
Researchers recruited 76 people, including individuals with SCAs (types 1, 2, 3, and 6, MSA-C, and healthy controls. Participants wore lightweight sensors on their wrists and ankles for one week while going about their normal routines at home.
Instead of focusing only on clinic-based tasks or just counting steps, these sensors used accelerometers to record the small “building blocks” of motion- called submovements– that make up everyday actions, such as lifting a hand or taking a step. Using machine learning (AI), the researchers analyzed features like speed, distance, and smoothness of these submovements to create a detailed picture of motor function.
What the Sensors Revealed
The data from wearable sensors captured meaningful patterns of movement that aligned with disease symptoms and progression.
• Strong Correlation with Clinical Scales: Sensor data from both the wrist and ankle closely matched scores from SARA and other clinical measures.
• Clear Separation from Controls: The AI models accurately distinguished between people with ataxia and healthy participants.
• Sensitive to Progression: Most importantly, the sensors detected disease progression, often more sensitively than clinical scales. As the disease progressed, submovements became smaller and slower, a change the sensors clearly captured.
• Reliable Data: The measurements were consistent across different days of the week, showing the system was robust.
• Broadly Applicable: Surprisingly, AI models that were originally trained on a different disease, amyotrophic lateral sclerosis (ALS), also worked well for tracking ataxia, suggesting this approach could be extended to monitoring other movement disorders.
Why wearable sensors matter
This study shows that wearable technology can accurately measure ataxia symptoms in the comfort of a person’s home. This represents a significant shift from limited, in-clinic tests to continuous, real-world monitoring. Key benefits are:
- Less patient burden by reducing the need for frequent clinic visits.
- Real-time data reflect how people function in daily life, not just in structured tests.
- Improved sensitivity to detect subtle changes missed by traditional rating scales.
- Stronger clinical trials, which could potentially require fewer participants or shorter durations, accelerating the path to new treatments.
For the ataxia community, this research offers hope for earlier interventions and more personalized care for faster progress toward therapies and a better quality of life.
Looking ahead
Earlier studies have used accelerometers in controlled settings, such as measuring gait or balance during walking tests. While useful, these task-based methods still capture only a limited snapshot of function. By moving to continuous, at-home monitoring, this study reflects the lived experience of patients more closely. It also highlights how approaches developed for one disease can inform research in another, as seen with the successful application of ALS-trained models. This shift from the clinic to the home represents a paradigm change in how researchers and clinicians approach rare neurological disorders.
Manohar and colleagues suggest several directions for future research:
- Larger patient groups to refine the models and ensure accuracy across different subtypes.
- More frequent monitoring (for example, every three months) to track changes with even greater precision.
- Testing in early or “pre-ataxic” stages, where current tools often fail to detect symptoms.
Despite lingering challenges, such as encouraging long-term participation and adapting models to each type of ataxia, this study lays the groundwork for wearable sensors to become a standard tool in ataxia care and research.
In Summary
SCAs and MSA-C are progressive diseases that urgently need better ways to measure change. While traditional rating scales have served as the primary tool for years, they have important limitations. This study demonstrates that wearable sensors worn at the wrist and ankle can fill this gap by providing sensitive, reliable, and real-world data on how symptoms progress. By harnessing familiar technology, researchers are opening the door to more efficient clinical trials and improved patient care. This represents a hopeful step for the ataxia community toward faster treatments and a better quality of life.
Conflict of Interest Statement
The author and editor have no conflicts of interest to declare.
Citation of Article Reviewed
Manohar. R., et al., At-home wearables and machine learning capture motor impairment and progression in adult ataxias. Brain, 2025, awaf154. (https://doi.org/10.1093/brain/awaf154)
Read Other SCAsource Summary Articles

24/7 Wearable Sensors: A New Way to Track Ataxia
Written by Poojashree Chettiar Edited by Pragya Goel, PhD AI and wearable tech may transform how ataxia is monitored Could everyday devices help track ataxia? Finding treatments for neurological disorders Read More…
Spinal Cord Damage Detected Prior to Disease Onset in Several SCAs
Written by Jacen Emerson Edited by Hannah Shorrock, PhD Human Imaging data reveals worsening spinal cord damage in several Ataxias that can begin before symptoms start. Why does the spinal Read More…

“¿De dónde vienes, adónde fuiste?”: Midiendo la progresión de la enfermedad en SCA1, 2, 3 y 6
Escrito por Alexandra PutkaEditado por Dr Hannah K ShorrockTraducido por Ismael Araujo-Aliaga Científicos caracterizan la progresión de las enfermedades SCA1, 2, 3 y 6, y descubren que los síntomas cambian Read More…



